Introduction
Within the realm of urology, many conditions are known to cause discomfort and distress to patients. One often overlooked but significant source of urological symptoms is pudendal nerve entrapment (PNE). PNE occurs when the pudendal nerve, responsible for sensory and motor functions in the pelvic region, becomes compressed or irritated. In this blog post, we will explore the causes, symptoms, diagnosis, and treatment options for pudendal nerve entrapment, shedding light on this frequently misunderstood condition.
Understanding the Pudendal Nerve
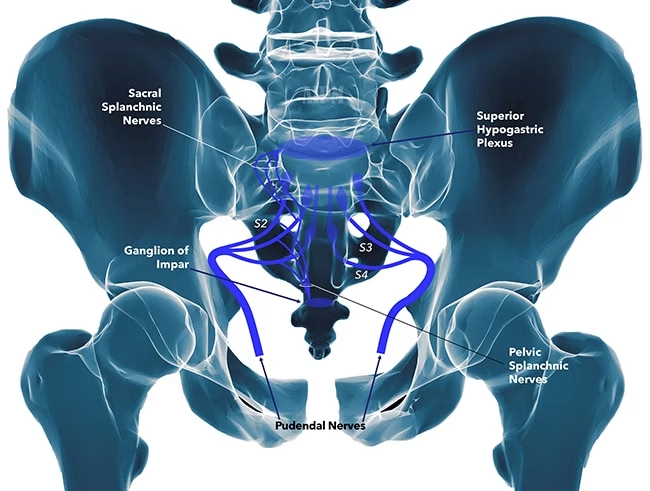
The pudendal nerve is a vital nerve in the pelvic region, responsible for providing sensation to the external genitalia, perineum, and rectum. Additionally, it plays a crucial role in controlling the muscles that are involved in urination, bowel movements, and sexual function. When the pudendal nerve becomes entrapped, patients may experience a variety of distressing symptoms.
Causes of Pudendal Nerve Entrapment
PNE can occur due to various reasons, including:
- Pelvic trauma or injury: Trauma to the pelvis, such as a fall or accident, can result in compression or entrapment of the pudendal nerve.
- Repetitive stress or overuse: Activities that put excessive pressure on the pudendal nerve, such as long-distance cycling, horseback riding, or sitting for prolonged periods, may lead to nerve compression over time.
- Post-surgical complications: Certain surgical procedures in the pelvic region, such as prostatectomy or hernia repair, can inadvertently damage or compress the pudendal nerve.
Symptoms of Pudendal Nerve Entrapment
The symptoms of PNE can manifest differently from person to person, but common complaints include:
- Chronic pelvic pain: This is the most prevalent symptom, characterized by persistent or recurring pain in the pelvic region, perineum, or rectum.
- Pain during sexual activity: Patients may experience pain or discomfort during sexual intercourse, affecting their overall quality of life and intimate relationships.
- Urinary and bowel dysfunction: PNE can lead to urinary urgency, frequency, or difficulty in initiating or maintaining urination. It may also cause constipation, incomplete bowel movements, or fecal incontinence.
Diagnosis and Treatment
Diagnosing PNE can be challenging due to its overlapping symptoms with other urological conditions. A thorough medical history, physical examination, and specialized diagnostic tests are essential for accurate diagnosis. These may include:
- Pudendal nerve block: An anesthetic injection near the pudendal nerve can temporarily relieve pain and confirm the involvement of the nerve in the patient’s symptoms.
- Electromyography (EMG) and nerve conduction studies: These tests assess the electrical activity and function of the pudendal nerve and surrounding muscles.
- Magnetic resonance neurography (MRN): This imaging technique can provide detailed images of the pudendal nerve and identify any anatomical abnormalities or compressions.
Once diagnosed, treatment options for PNE may include:
- Physical therapy: Pelvic floor physical therapy, including stretching, relaxation exercises, and biofeedback, can help alleviate symptoms and improve muscle function.
- Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs), neuropathic pain medications, and muscle relaxants may be prescribed to manage pain and reduce inflammation.
- Nerve decompression surgery: In severe cases of PNE that do not respond to conservative treatments, surgical release or decompression of the entrapped nerve may be considered.
Conclusion
In conclusion, pudendal nerve entrapment can have a profound impact on urological health. The compression or entrapment of the pudendal nerve can lead to symptoms such as urinary urgency, frequency, and incontinence. Additionally, it can cause sexual dysfunction, including pain during intercourse (dyspareunia), erectile dysfunction, and diminished genital sensation. These symptoms can significantly impair a person’s quality of life and require appropriate evaluation and management within the field of urology.